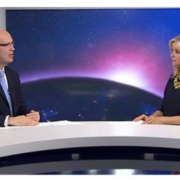
Without adequate care, pregnancy and childbirth are the number one cause of death and illness for women during humanitarian crises. Photo by EU/ECHO/Pierre Prakash.
There are now around 2,000 asylum seekers from Myanmar and Bangladesh seeking humanitarian assistance in Aceh. The Indonesian government and civil society must provide the healthcare they need, and it must include access to maternal and reproductive health services for the estimated 500 women among them. In humanitarian crises, pregnancy and childbirth are the number one cause of illness and death for women if adequate care is not available.
The Indonesian government has already agreed to provide assistance to the Rohingya asylum seekers for 12 months from May 2015, but it remains unclear how this assistance will be given and who will fund it.
Healthcare for asylum seekers in Aceh is poorly organised and does not meet international standards for reproductive health in humanitarian crises. The asylum seekers have been in Aceh since May – almost three months now – yet there is still no integrated action plan that brings all the different players involved together. Reproductive and maternal healthcare is ad hoc so far – each group operates separately, and there is little coordination.
These conditions result in assistance that is not required or inappropriate, and organisations doubling up. Some types of aid are overlooked altogether. Unfortunately, maternal and reproductive healthcare often falls in this category.
The Reproductive Health Response in Crisis Consortium (RHRC), a group formed by various UN agencies, governments, and nongovernmental organisations, has developed a Minimum Initial Service Package (MISP) for women’s healthcare in crises. The RHRC argues that failure to implement the package will increase maternal and neonatal deaths, violence against women, and sexually-transmitted diseases, including HIV/AIDS. It will also cause more unintended pregnancies and abortions. Without coordinated assistance from health professionals, pregnant women and women in childbirth are much more likely to encounter complications such as haemorrhage, eclampsia, and infection. Newborn babies, too, are more vulnerable to illness and death if no health worker is there to assist with their birth and make sure they begin breathing normally.
To prevent these negative outcomes, government and civil society stakeholders involved in providing healthcare to the Rohingya should follow the RHRC service package model. Pregnant women must have access to full antenatal care and delivery assistance – the government must ensure there are enough doctors and midwives, medicines and equipment, and must develop a strong referral system capable of referring pregnant women to government health clinics (puskesmas), and from clinics to hospitals. And care must not be limited to pregnant women. All women and girls need access to reproductive healthcare.
Safe places for women and girls must also be available. They need a place where they can gather without men and be safe from the threat of violence and sexual harassment. This is a vital part of humanitarian assistance, as sexual assault and rape are far more likely to occur during times of societal upheaval.
What remains to be explained is how the Indonesian government will pay for assistance given to asylum seekers in Aceh. Who will be responsible for it? Since the asylum seekers have landed and are being cared for in many different parts of Aceh, the provincial government has no choice but to take responsibility for relief coordination, developing an integrated action plan, and funding. Local governments, meanwhile, should implement the provincial plan and be the day-to-day face of assistance.
There are still many questions that need to be answered. If a pregnant woman gives birth at a puskesmas, who will pay for her? Who will be responsible for her? Will she receive government support to become a member of the national insurance scheme (Jaminan Kesehatan Nasional) or the Acehnese health insurance scheme (Jaminan Kesehatan Aceh)? Will the puskesmas elect not to charge her for its services? Will the local government give the puskesmas additional funds to cover the money lost through providing services to asylum seekers? What if a woman needs a caesarean section to give birth safely? Or if her baby needs hospital care?
The national, provincial and local governments must also consider the impact that healthcare policies for asylum seekers might have on the local population. As mentioned, Aceh already has a provincial health insurance scheme that covers healthcare costs for the province’s residents. If healthcare given to asylum seekers is incorporated into the existing public healthcare system, using existing facilities and staff, there should be no negative impact for the Acehnese people. In reality, the number of asylum seekers is not big enough for health clinics to be overrun by requests for services, nor of asylum seekers receiving care not given to Acehnese locals, but this needs to be explained to the public.
In fact, all these issues need to be discussed by all stakeholders, and solutions must be found – quickly. The time-based nature of pregnancy means that female asylum seekers cannot wait for the government to make decisions.