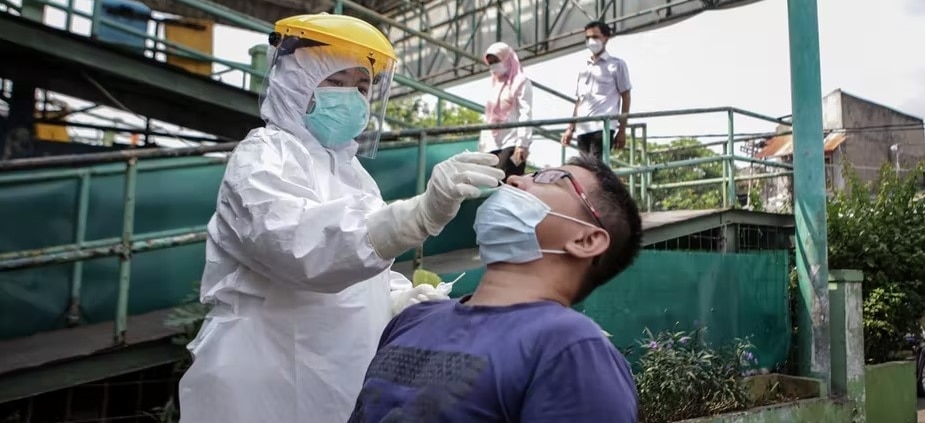
Indonesia has handled the Omicron wave much better than it did the Delta wave in 2021. Photo by Fauzan for Antara.
Indonesia is emerging from another surge in Covid-19 infections. Since the first case of Omicron was confirmed in early December 2021, Indonesia has recorded more than 1.5 million new cases and 7,400 deaths.
This data is far less daunting compared to Indonesia’s experience with the Delta wave in 2021, when more than 2.5 million Indonesians were infected, and more than 112,000 deaths were recorded. The health system has also coped better this time around. The bed occupancy rate remained steady at around 60% during the Omicron peak – a stark contrast with the situation in July and August 2021, when hospitals were unable to cope with the Delta surge and high mortality rates were recorded among health workers.
There are several reasons for the seemingly better outcomes with this surge. The first is the less severe clinical presentation of the Omicron variant compared to Delta. Second, more Indonesians have now received vaccinations. At the time of writing, more than 90% of the population had received at least one dose and more than 70% were fully vaccinated. Vaccine coverage is higher still in Java and Bali, where booster shots have been rolled out for the general population since the end of January.
Further, widespread previous infection appears to have provided some degree of immunity against the Omicron surge. A serological survey conducted in November and December 2021 found that 86% of Indonesians already had antibodies against Covid-19 (this was at a time when average vaccination coverage was only 59% for dose one and 42% for two doses).
The Indonesian health system has also learnt from previous waves. The Ministry of Health implemented a more effective surveillance system and ensured higher testing capacity before Omicron peaked. Local health centres (puskesmas) were ready to lead with case recording and local tracing and testing, there were almost no stockouts of rapid tests, and PCR testing capacity kept up with demand. There was also better readiness at the health facility level in terms of anticipating for a surge in cases. Similarly, the government acted quickly to adjust travel restrictions and quarantine requirements.
The government was clearly buoyed by its ability to manage the Omicron wave. By the second week of March, despite a record number of daily new cases at 26,000, Indonesia began loosening social restrictions. Quarantine for international travellers was reduced from three days to just one (and on 21 March dropped altogether). The mandatory PCR or rapid antigen swab test requirement for domestic flights and train travel was scrapped for passengers with at least two shots of the vaccine. Confusingly, however, the Ministry of Home Affairs at the same time encouraged a reintroduction of social restrictions in many districts of Java and Bali. Although the government is still promoting its “5M” health protocols (hand washing, masks, social distancing, avoid crowds, reduce mobility), the public have begun questioning when Indonesians will follow in the footsteps of other European countries and start removing their masks.
But there are plenty of reasons for caution. The first is that Omicron is still around, and it remains 3.2 times more transmissible than Delta. During the Omicron peak there were about 63,000 new cases per day, compared to 56,000 during the Delta wave. Indonesia was lucky that the peak was not more severe and its health systems were not overwhelmed. The BA.2 sub-variant of Omicron has led to recent record high spikes in cases in the UK and has already been identified in Indonesia. The WHO has said that while the severity of disease appears similar to the BA.1 sub-variant, BA.2 is much more transmissible. Its full impact is yet to be felt in Indonesia.
Second, geographical disparity in vaccine coverage is a serious issue. At the end of January 2022, there were 19 provinces where less than 50% of the population had received two doses of vaccine. Meanwhile, provinces prioritised because of their disease burden or economic significance have achieved almost universal coverage. Even by mid-March 2022, in eastern provinces such as Papua, West Papua, Maluku and North Maluku, the proportion of the population that had received two doses of vaccine ranged from just 27 to 46%. This is significantly lower than the national average (73%), and far below provinces like Jakarta (124%) and Bali (104%).
Immunity levels, whether acquired through vaccination or infection, wane over time. If vaccine inequality is not addressed quickly, areas with low vaccination coverage could experience a much higher case load and mortality rates if another wave hits.
Another cause for concern is fatigue with public health measures like mask wearing, social distancing and social isolation. Prominent Universitas Indonesia epidemiologist Pandu Riono has stated that social restrictions known as PPKM may no longer be as effective, as Indonesians are getting fed up with the intermittent restrictions on activities.
Like many people around the world, Indonesians are longing for some normalcy, including in their daily social interactions and travel. More lax mask wearing and social distancing measures could result in much higher cases and mortality if another wave strikes.
How can Indonesia get the balance right?
Indonesia first needs to ensure it implements a strong risk communication strategy. Easing of travel restrictions and quarantine requirements should not be interpreted as giving the green light to a complete relaxation of public health measures. People who have been fully vaccinated should continue to wear masks in public, limit mobility and avoid gathering in crowds. The arrival of the BA.2 variant in Indonesia suggests the government needs to start stressing the importance of restricting mobility ahead of the Eid holiday in early May.
Consistent public health messaging is required, and not just by the government. The media must resist the temptation to use sensationalist headings and framing that could mislead the public.
Second, the government needs to remain alert and responsive to any further Covid-19 spikes overseas. Restrictions for international travel should be tightened as soon as there are suspicions of new variants emerging in other countries. The strict quarantine requirements during November and December 2021 (which required international travellers to undergo a mandatory 10 days of quarantine) appeared to be somewhat effective in delaying the arrival of the Omicron wave and bought Indonesia precious time to increase its vaccination coverage.
Finally, and most crucially, health system resilience is at the core of mitigating the risks of the pandemic in the future and ensuring that other essential health services remain accessible to those in need. The Covid-19 pandemic in Indonesia resulted in significant disruptions to other vital health services, including for pregnant women, newborns, and those with chronic illnesses such as heart disease and cancer. Some puskesmas closed or reduced their operating hours, while some hospitals were converted into Covid-19 facilities. Mobility restrictions meant that some sick people were prevented from accessing health facilities.
Creating a more resilient health system will require more intensive collaboration with health education institutions to handle future surges in need for human resources. The past two years have shown that health sector students can play a critical role in filling workforce gaps, and in the rapid scaling up of vaccination and testing and tracing.
Strengthening service delivery is also vital, including by working with private sector and community initiatives to anticipate future spikes. This could entail ensuring that quality telemedicine is provided by both the public and private sectors and that both public and private hospitals continue to receive Covid-19 patients during peak periods. Better coordination with community initiatives could support patients to self-isolate and promote compliance with social restrictions at the community level.
Finally, village level officials are uniquely positioned to respond to community needs. They have access to village funds (dana desa) and are often well connected to their local communities. Local governments must put greater effort into empowering and supporting village officials so that village funds are directed toward supporting community responses to the pandemic.
Indonesia has done much better in handling Omicron than it did with Delta, but that is no reason for complacency. Indonesians are weary of restrictions, but in a country with unequal vaccination coverage and a stretched health system it is too soon to abandon masks and social distancing.