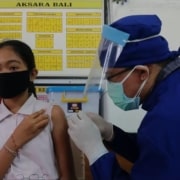
Breast and cervical cancer are the leading causes of cancer-related deaths among Indonesian women but low cost cervical cancer screening is only available in eight of Indonesia’s 34 provinces. Photo by Kristopher Radder for US Pacific Fleet.
Cancer presents enormous challenges to health systems in low- and middle-income countries like Indonesia. The country is experiencing a health transition. Deaths from communicable diseases are on the decline, while mortality and suffering from chronic diseases such as cancer are rapidly escalating. This reflects changing lifestyles, poor environmental conditions, shifting consumption patterns and the low capacity of health care systems to provide cancer prevention, screening and treatment.
In low- and middle-income countries, the mortality rate from cancer is unacceptably high – much higher than in wealthier countries. For example, more than 270,000 women die from cervical cancer every year, with more than 85 per cent of these deaths occurring in low- and middle-income countries. This gap in the global burden of cancer is now referred to as “the cancer divide”. It can only be addressed by strengthening the capacity of health systems in low and middle income countries to provide cancer prevention, screening and treatment services.
In Indonesia, cancer is now one of the top five causes of adult mortality and breast and cervical cancer are the leading causes of cancer-related deaths among Indonesian women. Yet low cost cervical cancer screening is only available in eight of Indonesia’s 34 provinces, and awareness and uptake of screening remains very low. There are also cultural barriers that reduce women’s willingness to undergo cervical examinations. These need to be better understood and accommodated if women’s access to life-saving cancer screening is to be increased.
Cervical cancer is triggered by the presence of the sexually transmitted human papillomavirus (HPV) and is a highly preventable condition. In 2014, more than 89 million women aged 15 years and older were at risk of developing cervical cancer in Indonesia, and about 20,000 new cervical cancer cases are diagnosed each year. It is likely this figure significantly underestimates the real incidence of cervical cancer, and does not match the very high rates of HPV infection among Indonesian women. This is because Indonesia is still establishing a national cancer registry, and many women with cervical cancer still do not seek treatment. Moreover, survival rates for women who do access cancer treatment are very poor, with only half of all Indonesian women diagnosed with cervical cancer surviving. This is mainly because of late diagnosis and poor access to treatment regimes.
Australia and many other high income countries now offer free vaccination for adolescents against HPV, dramatically reducing the number of adults who will develop cervical and other cancers caused by HPV. Indonesia is seeking to generate the evidence base needed for the introduction of free universal HPV vaccination. While this process may be protracted, it has begun and involves close collaboration between researchers at the University of Melbourne, Gadjah Mada University in Yogyakarta, and the University of Indonesia in Jakarta. A pilot project was launched this month, with funding provided by the Indonesian Directorate General of Higher Education. The project will examine biological, epidemiological and social factors over 18 months in Central Java, to determine exactly what is needed for a pilot HPV vaccination program.
The project is investigating women’s and men’s knowledge and attitudes towards HPV, HPV vaccination, cervical cancer, and cervical cancer screening, as well as women’s behaviour in relation to contracting HPV and screening for cervical cancer. Low and incorrect knowledge of the risks of both HPV and cervical cancer are constraining women’s access to vaccination and screening. In particular, the relationship between HPV and cervical cancer is very poorly understood. Widespread community education will be required if the uptake of both prevention and screening programs is to improve.
When an Indonesian woman does seek out biomedical care, and is diagnosed with cervical cancer her family and community will typically rally to offer support and raise money for treatment. This is a very different scenario to other Asian countries such as India and Bangladesh, where women suffering from cervical and breast cancer are often ostracised and even ejected from their families. It appears that HPV and cervical cancer are viewed at the community level by Indonesians as conditions that anyone can develop, and therefore lack the stigma attached to other sexually transmissible infections such as HIV. This new research seeks to confirm these positive attitudes and understand how they might be used to promote cancer screening and HPV vaccination.
The inclusion of both women and men in the research and subsequent interventions is crucial. As men are also carriers of HPV, their awareness of the risk of cervical cancer is critical to prevention. Men are also important decision makers with regards to vaccination of their children and women’s access to preventative screening for cervical cancer. Including men and women equally is a significant departure from the typical women-focused approach to reproductive health in Indonesia. HPV is also involved in anal and oropharyngeal cancer, which equally affect men and women.
While this study is focused on the end game of establishing free HPV vaccination, there is also much still to be learnt about cancer screening and the experiences of those Indonesian women who undergo cancer treatment and live with the disease. It is hoped that such knowledge could make a real contribution toward closing the gap in cancer outcomes for women in low- and middle-income countries.
The pilot project is titled “Surveillance of the Burden of HPV Infection and HPV Type-specific Distribution in Purworejo, Indonesia: Implications for a Cervical Cancer Prevention Strategy.” Dr Linda Rae Bennett and PhD candidate Belinda Spagnoletti of the Nossal Institute for Global Health at the University of Melbourne are leading the social research component of the study. Professor Siswanto Wilopo, director of the Centre for Reproductive Health at Gadjah Mada, will head the epidemiological component of the research and Associate Professor Sepher Tabrizi from the Women’s Centre for Infectious Diseases at The Royal Women’s Hospital will support the biological analysis. The goal is to develop a low-cost, population-specific vaccine for the prevention of high risk HPV strands in Indonesia.